December 3, 2024
World AIDS Day, observed every year on December 1, is a time to honour the lives of those affected by HIV and AIDS, remember those lost, and reflect on the ongoing efforts to address HIV. It is an important day to highlight the ways that science developments are providing new opportunities to prevent, diagnose and treat HIV.
HIV in Canada
HIV diagnosis rates in Canada were relatively stable from 2013 to 2019. Although diagnosis rates declined in 2020, it was likely due to reduced access to HIV testing services as a result of the COVID-19 pandemic. Since 2021, HIV diagnosis rates in Canada have been steadily increasing, reaching a ten-year peak of 6.1 per 100,000 people in 2023.
Figure 1 - HIV in Canada: 2023 surveillance highlights
-
Figure 1 - HIV in Canada: 2023 surveillance highlights - Text version
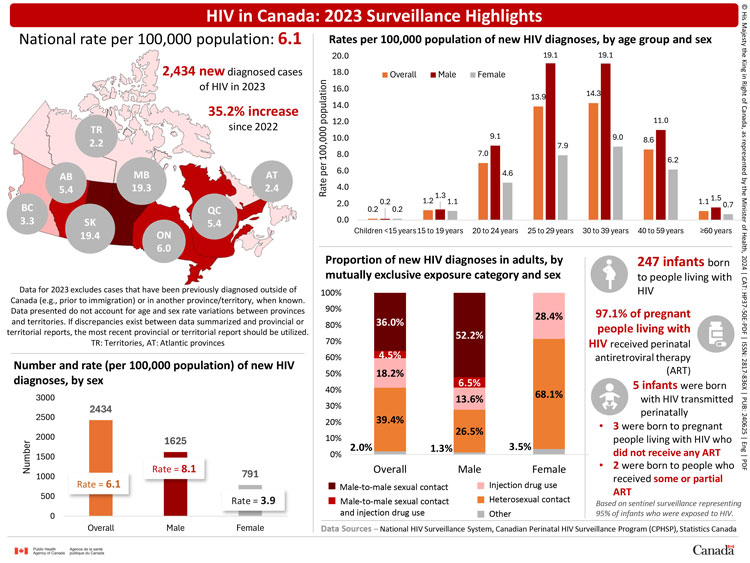
HIV in Canada: 2023 surveillance highlights
- 2,434 new HIV diagnoses in 2023 (35.2% increase since 2022)
- National rate of new HIV diagnoses for 2023 – 6.1 per 100,000 population
2023 Data Notes
- Data for 2023 excludes cases that have been previously diagnosed outside of Canada (e.g. prior to immigration) or in another province/territory, when known.
- Data presented do not account for age and sex rate variations between provinces and territories.
- If discrepancies exist between data summarized and provincial or territorial reports, the most recent provincial or territorial report should be utilized.
- TR: Territories, AT: Atlantic provinces
New diagnosis rate per 100,000 population in 2023, by province or territory
- Provincial and territorial HIV diagnosis rates:
- Territories – 2.2
- British Columbia – 3.3
- Alberta – 5.4
- Saskatchewan – 19.4
- Manitoba – 19.3
- Ontario – 6.0
- Quebec – 5.4
- Atlantic – 2.4
Number and rate (per 100,000 population) of new HIV diagnoses, by sex
- 1,625 new HIV diagnoses in males – Rate of 8.1
- 791 new HIV diagnoses in females – Rate of 3.9
Rates per 100,000 population of new HIV diagnoses, by age group and sex
- Overall:
- Children <15 years of age – 0.2
- 15-19 years of age – 1.2
- 20-24 years of age – 7.0
- 25-29 years of age – 13.9
- 30-39 years of age – 14.3
- 40-59 years of age – 8.6
- ≥60 years of age – 1.1
- In males:
- Children <15 years of age – 0.2
- 15-19 years of age – 1.3
- 20-24 years of age – 9.1
- 25-29 years of age – 19.1
- 30-39 years of age – 19.1
- 40-59 years of age – 11.0
- ≥60 years of age – 1.5
- In females:
- Children <15 years of age – 0.2
- 15-19 years of age – 1.1
- 20-24 years of age – 4.6
- 25-29 years of age – 7.9
- 30-39 years of age – 9.0
- 40-59 years of age – 6.2
- ≥60 years of age – 0.7
Distribution of new HIV diagnoses, by mutually exclusive exposure category and sex
- Overall:
- Male-to-male sexual contact – 36.0%
- Male-to-male sexual contact and injection drug use – 4.5%
- Injection drug use – 18.2%
- Heterosexual contact – 39.4%
- Other – 2.0%
- In males:
- Male-to-male sexual contact – 52.2%
- Male-to-male sexual contact and injection drug use – 6.5%
- Injection drug use – 13.6%
- Heterosexual contact – 26.5%
- Other – 1.3%
- In females:
- Injection drug use – 28.4%
- Heterosexual contact – 68.1%
- Other – 3.5%
Perinatal HIV Surveillance in 2023
- 247 infants born to people living with HIV.
- 97.1% of pregnant people living with HIV received perinatal antiretroviral therapy (ART).
- 5 infants were born with HIV transmitted perinatally: 3 were born to pregnant people living with HIV who did not receive any ART, and 2 were born to people who received some or partial ART.
- Based on sentinel surveillance representing 95% of infants who were exposed to HIV.
Data Sources
National HIV Surveillance System (HASS), Canadian Perinatal HIV Surveillance System (CPHSP), Statistics Canada
The reasons behind the recent increase in HIV diagnoses are complex. Infection rates are influenced by social determinants of health such as housing insecurity, low income, substance use, experiences of violence, living in rural or remote areas and limited access to health care.
HIV can affect anyone. The good news is thanks to advances in science and medicine, there are now many ways to prevent HIV. Each person can choose the prevention method that best supports their health and well-being.
Modern advances in HIV testing

Dr. Theresa Tam, Chief Public Health Officer of Canada, taking an HIV self-test kit.
Knowing your HIV status is the first step to prevention, treatment and care.
HIV self-test kits are a modern advancement that provide accessible testing and offer a safe, reliable, anonymous and confidential way for people to learn your HIV status. They are the first and self-tests authorized in Canada for an infectious disease.
A range of testing options, including anonymous testing, continue to remain available across Canada and are delivered in public health and community settings.
Find a testing location near you and learn more about HIV self-testing.
Treatment as Prevention: Undetectable=Untransmittable (U=U)
Stigma and discrimination are significant barriers that prevent people from getting tested or accessing the care, treatment and support they need. Undetectable=Untransmittable (U=U) is an initiative that is changing what it means to live with HIV by reducing the stigma and discrimination attached to the diagnosis.
U=U is a movement dedicated to promoting the scientific evidence that shows HIV is not passed on through sex when a person living with HIV is receiving treatment and the amount of HIV in their blood remains low.
U=U is a key tool in preventing new cases of HIV, reducing HIV stigma and supporting the health and well-being of people living with HIV. In November 2023, the Healthy Canadians podcast released an episode featuring an in-depth conversation about U=U. When asked about the impact of U=U on people living with HIV, Adrian Betts, Executive Director of the AIDS Committee of Durham region explained, “But what it also does (sic) is dismantle stigma, and give people living with HIV an incredible sense of comfort that they’ve never had before. I don’t know a single person living with HIV who ever—whose biggest anxiety is not about infecting somebody else. So, it was viewed as a game changer in many ways.”
Figure 2 - HIV positive. Living Positive

HIV treatment helps people living with HIV to stay healthy and can prevent it from being passed on.
-
Figure 2 - HIV positive. Living Positive - Text version
HIV Positive. Living Positive.
The science is clear.
HIV treatment helps people living with HIV to stay healthy and can prevent it from being passed on.
Canada.ca/HIV
Use of HIV PrEP & HIV PEP can reduce risk of HIV infection
There are also new medications available for individuals who do not have HIV but engage in activities that have increased risk of exposure to HIV. HIV Pre-Exposure Prophylaxis (PrEP) is a medication that is taken on an ongoing, regular basis to prevent an HIV infection. HIV Post-Exposure Prophylaxis (PEP) is another medication that can be taken after a high-risk exposure to HIV, ideally within 72 hours, to prevent infection. HIV PEP is intended for use following a single specific exposure.
Learn more about HIV PrEP and PEP.
